Insurance companies deal with a lot of information, especially when it comes to claims. Think about all the details from each claim filed – who was involved, what happened, how much was lost. Making sense of all that data is where claims data analytics insurance comes into play. It’s basically using smart tools to look at that information and find patterns, spot problems, and generally make things run smoother. This isn’t just about crunching numbers; it’s about using what you learn to make better decisions across the board, from figuring out if a claim is legit to improving how customers are treated.
Key Takeaways
- Claims data analytics insurance helps insurers understand claim patterns, detect fraud, and improve processes by analyzing vast amounts of information.
- Using claims data helps in preventing losses and reducing risks by identifying trends and potential issues before they become major problems.
- Advanced techniques like predictive modeling and machine learning can forecast claim severity and identify unusual activities, leading to more accurate outcomes.
- Insights from claims data can refine underwriting, leading to more precise risk assessment and better pricing strategies for insurance products.
- Analyzing claims data can improve the customer experience by speeding up settlements and personalizing interactions, while also boosting operational efficiency.
Leveraging Claims Data Analytics in Insurance
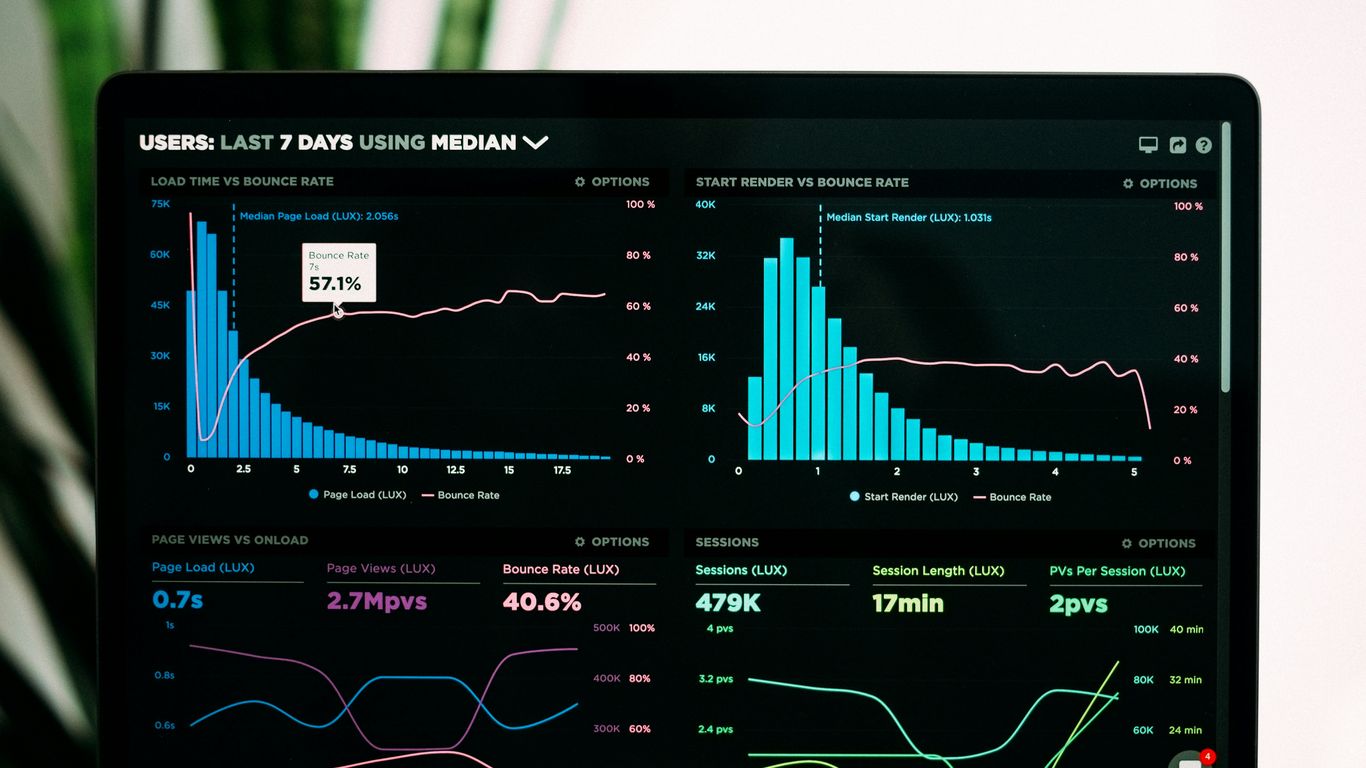
Understanding the Role of Claims Data
Claims data is the lifeblood of an insurance company. It’s not just about tracking payments; it’s a rich source of information about what’s happening in the real world. Every claim filed, from a minor fender bender to a major property damage event, tells a story. This data can reveal trends in accidents, the effectiveness of safety measures, and even emerging risks that we might not have considered before. By analyzing this information, insurers can get a much clearer picture of their exposure and how well their policies are performing. It’s like having a direct line to the experiences of your policyholders, offering insights that can shape everything from product development to customer service. Understanding the patterns within this data is key to making smarter business decisions.
The Evolution of Claims Analytics
Claims analytics hasn’t always been as sophisticated as it is today. In the past, it was mostly about basic reporting – how many claims were filed, how much was paid out, and how long it took to settle. Think simple spreadsheets and manual calculations. But things have changed. With advancements in technology and the sheer volume of data now available, we’ve moved into a new era. We’re now using advanced tools to predict future losses, identify potentially fraudulent claims before they’re paid, and even pinpoint areas where our claims processes could be smoother. This evolution means we’re not just reacting to claims anymore; we’re becoming more proactive. It’s a shift from just managing claims to truly understanding and optimizing the entire claims lifecycle. This journey has been driven by the need for greater efficiency and accuracy in insurance operations.
Strategic Importance of Claims Data Analytics
Looking at claims data isn’t just an operational task; it’s a strategic imperative. The insights gained can directly impact an insurer’s bottom line and its long-term viability. For instance, identifying patterns in claims can help refine underwriting guidelines, leading to more accurate pricing and better risk selection. It also plays a huge role in managing financial exposure. By understanding loss trends and potential future claims, companies can better manage their reserves and capital. This proactive approach helps prevent situations where an insurer might not have enough funds to cover its obligations, which is critical for maintaining solvency. Ultimately, effective claims analytics allows insurers to be more competitive, more resilient, and better positioned to serve their customers in an ever-changing risk landscape.
Foundational Elements of Claims Data Analytics
Before diving into the advanced applications of claims data analytics, it’s important to get the basics right. This means understanding where your data comes from, making sure it’s clean and usable, and knowing what metrics actually matter. Without these foundational pieces, any analytics effort is likely to falter.
Data Sources and Collection
Claims data doesn’t just appear out of thin air. It’s gathered from a variety of places, and each source has its own quirks. Think about the initial notice of loss, which might come through a phone call, an online portal, or even an agent. Then there’s the information gathered during the investigation phase: police reports, repair estimates, medical records, witness statements – the list goes on. Each piece of information needs to be captured accurately and efficiently. The goal is to create a unified view of the claim, pulling data from all these disparate points.
Here are some common sources:
- First Notice of Loss (FNOL) Systems: Captures initial claim reporting.
- Claims Management Systems: Stores detailed claim information, adjuster notes, and financial transactions.
- Policy Administration Systems: Provides context on coverage, limits, and deductibles.
- External Data Providers: Such as weather data, geographic information, or public records.
- Third-Party Administrators (TPAs): If claims are outsourced.
Getting this data into a usable format is the first hurdle. It often involves integrating different systems and standardizing formats. For instance, a police report might be a PDF, while a repair estimate could be an Excel file. Making sense of it all requires careful planning and often some technical heavy lifting. You can find more on the claims process itself here.
Data Quality and Preparation
Raw data is rarely perfect. It’s often messy, incomplete, or inconsistent. Before you can do any meaningful analysis, you need to clean and prepare your data. This involves several steps:
- Validation: Checking if the data makes sense. For example, are dates logical? Are amounts within expected ranges?
- Cleansing: Correcting errors, filling in missing values where possible, and removing duplicates.
- Standardization: Ensuring data is in a consistent format across all sources. This might mean converting dates to a single format or standardizing address fields.
- Transformation: Restructuring data to make it suitable for analysis, perhaps by creating new variables or aggregating existing ones.
Poor data quality is a silent killer of analytics projects. If the data you’re feeding into your models is flawed, the insights you get will be equally flawed, leading to bad decisions and wasted resources. It’s better to spend more time upfront ensuring data integrity than to chase inaccurate conclusions later.
This preparation phase can be time-consuming, but it’s absolutely critical. Think of it like preparing ingredients before cooking; you can’t make a great meal with rotten vegetables.
Key Performance Indicators for Claims
To measure the effectiveness of your claims process and analytics efforts, you need to track the right metrics. These Key Performance Indicators (KPIs) provide a snapshot of how well things are running and where improvements are needed. They help you understand not just what is happening, but why.
Here are some essential KPIs:
- Claim Cycle Time: The average time it takes to close a claim from the date it’s reported. Shorter cycle times usually mean happier customers and lower costs.
- Loss Ratio: The ratio of claims paid out (plus reserves) to premiums earned. This is a fundamental measure of profitability.
- Indemnity Spend: The total amount paid out for covered losses. Tracking this helps understand claim severity.
- Expense Ratio: The cost of handling claims (adjuster salaries, operational costs) as a percentage of premiums.
- Customer Satisfaction (CSAT) Scores: Direct feedback from policyholders on their claims experience.
- Fraud Detection Rate: The percentage of claims identified as fraudulent. This indicates the effectiveness of your fraud prevention measures.
These indicators give you a clear picture of performance. For example, if your claim cycle time is increasing, it might point to inefficiencies in your investigation or settlement process. Analyzing these KPIs regularly helps you identify trends and make data-driven adjustments to improve claims handling.
Core Applications of Claims Data Analytics
Claims data analytics isn’t just about looking backward; it’s about making the present and future of insurance operations much smoother and smarter. When we talk about core applications, we’re really focusing on the day-to-day, high-impact uses that directly affect an insurer’s bottom line and its relationship with policyholders. It’s where the rubber meets the road, so to speak.
Fraud Detection and Prevention
This is a big one. Insurance fraud costs the industry billions every year, and those costs get passed on to everyone through higher premiums. Analytics can spot patterns that human eyes might miss. Think about claims that look too similar, or claimants who have a history of suspicious activity. By sifting through vast amounts of data, algorithms can flag potentially fraudulent claims for further investigation. This isn’t about accusing everyone, but about identifying outliers that warrant a closer look. It helps protect the integrity of the insurance pool and keeps costs down for honest policyholders.
- Identifying duplicate claims across different insurers.
- Flagging claims with unusual repair estimates or medical billing.
- Detecting staged accidents or suspicious injury patterns.
The goal is to build robust systems that can identify anomalies without creating undue burden on legitimate claimants. It’s a delicate balance, but analytics provides the tools to achieve it.
Loss Prevention and Risk Mitigation
Beyond just paying out claims, analytics helps insurers get proactive. By analyzing historical claims data, insurers can identify trends and common causes of loss. For example, if data shows a spike in water damage claims in a certain region during specific weather events, an insurer can work with policyholders in that area to offer advice or resources on preventing such damage. This could involve recommending specific maintenance practices or even offering discounts for installing preventative measures. It’s about shifting from a reactive model to a more proactive one, helping policyholders avoid losses in the first place. This benefits everyone involved, reducing claim frequency and severity. It’s a key part of understanding the claims process.
Claims Process Optimization
Nobody likes a drawn-out claims process. Analytics can streamline operations significantly. By examining every step of the claims journey, from initial notice to final settlement, insurers can pinpoint bottlenecks. Are certain types of claims taking longer to process? Are adjusters spending too much time on administrative tasks? Data can reveal these inefficiencies. Automating routine tasks, improving communication workflows, and better allocating resources based on claim complexity are all outcomes of this analysis. The aim is to make the process faster, more consistent, and less frustrating for the policyholder, while also improving the efficiency of the claims department.
| Process Step | Average Time (Days) | Potential Bottleneck Identified | Optimization Strategy |
|---|---|---|---|
| Notice of Loss | 1.5 | No | N/A |
| Initial Assignment | 0.8 | No | N/A |
| Investigation | 15.2 | Yes | AI-assisted document review, virtual inspections |
| Coverage Determination | 4.1 | No | N/A |
| Valuation | 10.5 | Yes | Standardized repair cost databases, expert systems |
| Settlement | 5.3 | No | N/A |
Advanced Analytics Techniques for Claims
Moving beyond basic reporting, advanced analytics techniques are really changing how we handle insurance claims. These methods let us dig deeper into the data, finding patterns and insights that weren’t visible before. It’s about using sophisticated tools to get a much clearer picture of what’s happening.
Predictive Modeling for Claims
Predictive modeling uses historical data to forecast future events. In claims, this means we can anticipate claim frequency, severity, and even potential fraud. By analyzing past claim details, we can build models that help estimate the likelihood of future claims and their potential costs. This helps in setting reserves more accurately and planning resources.
- Forecasting Claim Volume: Predicting how many claims to expect in a given period.
- Estimating Claim Severity: Projecting the average cost of claims.
- Identifying High-Risk Claims: Flagging claims that are more likely to be complex or fraudulent.
This kind of foresight is a game-changer for financial planning and resource allocation. It allows insurers to be more proactive rather than just reactive to claim events.
Natural Language Processing in Claims
Lots of claim information comes in unstructured text – think adjuster notes, police reports, or customer emails. Natural Language Processing (NLP) helps us make sense of all that text. It can extract key information, categorize documents, and even gauge sentiment from customer communications. This speeds up the review process and ensures important details aren’t missed.
NLP can help with:
- Analyzing adjuster notes for consistency and completeness.
- Extracting details from unstructured documents like medical reports.
- Categorizing claim types based on initial descriptions.
It’s like having a super-fast assistant that can read and understand vast amounts of text data. This is particularly useful when reviewing policy language to determine coverage, a process that can take weeks for human experts understanding the role of claims data.
Machine Learning for Anomaly Detection
Machine learning algorithms are excellent at spotting things that are unusual or don’t fit the normal pattern. In claims, this is invaluable for fraud detection. Anomaly detection can flag claims that have unusual characteristics, such as inconsistent details, suspicious timing, or abnormal repair costs, which might indicate fraudulent activity. It works by learning what ‘normal’ looks like and then highlighting deviations.
The goal here isn’t just to catch fraud after it happens, but to build systems that can identify suspicious patterns early on. This proactive approach can save significant amounts of money and protect honest policyholders.
These advanced techniques, when applied thoughtfully, can transform claims operations from a cost center into a strategic advantage. They allow for more precise risk assessment, better resource management, and ultimately, a more efficient and effective claims process.
Enhancing Underwriting with Claims Insights
Refining Risk Assessment
Claims data offers a direct look at what actually happens after a policy is issued. It’s a goldmine for underwriters trying to get a clearer picture of risk. Instead of just relying on application data, which can sometimes be a bit optimistic, claims history shows the real-world outcomes. We can see which types of properties have more water damage claims, or which driver profiles tend to have more accidents. This kind of information helps us move beyond broad categories and really pinpoint specific risks. For example, analyzing claims related to a particular type of business operation can reveal hidden exposures that weren’t obvious during the initial application. This detailed view allows for more precise risk classification, moving away from generalized assumptions.
- Claims data provides a feedback loop for underwriting accuracy.
- It helps identify emerging risk trends before they become widespread.
- Analyzing claim frequency and severity for specific demographics or property types can refine risk models.
By digging into the details of past claims, underwriters can build a more robust understanding of potential future losses. This isn’t about penalizing policyholders; it’s about accurately pricing risk and ensuring the long-term health of the insurance pool.
Pricing Accuracy and Segmentation
Once we have a better handle on risk assessment, we can talk about pricing. Claims data lets us segment policyholders more effectively. If a certain group of policyholders consistently has fewer and less severe claims, they should logically pay less. Conversely, those with a higher claims history might face higher premiums or require specific risk management measures. This granular approach to pricing is fairer to the customer and better for the insurer’s bottom line. It moves us closer to a true pay-as-you-go model, where premiums reflect actual risk exposure. This also helps in identifying profitable market segments and areas where pricing might need adjustment. For instance, claims data analytics can highlight geographic areas with increasing weather-related claims, prompting a review of pricing for properties in those zones.
Portfolio Performance Analysis
Looking at claims data across an entire portfolio provides a bird’s-eye view of performance. We can see which lines of business are performing well and which are struggling. Are we seeing an uptick in liability claims for a specific industry? Is a particular product line experiencing higher-than-expected losses? This high-level analysis helps in making strategic decisions about which markets to grow, which to retrench from, and where to invest in loss prevention efforts. It’s about understanding the overall health of the insurance book and making adjustments to maintain profitability and stability. For example, a review of claims might show that a particular type of commercial policy is consistently unprofitable, leading to a decision to revise its terms or discontinue it. The investigation process for claims provides the raw data for this analysis.
Improving Customer Experience Through Analytics
Insurers are increasingly turning to data analytics to get a better handle on what policyholders actually need and want. It’s not just about processing claims faster, though that’s a big part of it. It’s about making the whole interaction feel smoother and more supportive. When a customer has to file a claim, it’s usually a stressful time. Using analytics helps insurers understand where the friction points are and how to smooth them out.
Streamlining Claims Settlement
Nobody likes waiting around for a claim to be processed. Analytics can speed this up significantly. By looking at historical claim data, insurers can identify patterns that lead to quicker settlements. This might involve automating parts of the process for simpler claims or flagging complex ones for immediate, specialized attention. The goal is to reduce the time from when a loss is reported to when the policyholder receives their payment. This involves a careful review of policy terms and the facts of the incident to determine coverage.
- Automate routine claim validation.
- Predict claim complexity for resource allocation.
- Identify and resolve bottlenecks in the workflow.
This focus on efficiency means less waiting and fewer follow-up calls for the customer. It’s about getting people back on their feet faster after a covered event. Understanding the steps in the insurance claims process helps pinpoint where analytics can make the biggest difference.
Personalizing Policyholder Interactions
Beyond just claims, analytics can help insurers communicate better with their customers throughout the policy lifecycle. By analyzing customer data, insurers can tailor communications, offers, and even policy recommendations. For instance, if a customer has recently experienced a specific type of loss, an insurer might proactively offer advice or relevant coverage adjustments. This moves the relationship from purely transactional to more of a partnership. It’s about anticipating needs rather than just reacting to them.
Personalized communication builds trust and loyalty. When customers feel understood and valued, they are more likely to stay with their insurer and recommend them to others.
Measuring Customer Satisfaction
Finally, analytics provides powerful tools for measuring how satisfied customers are. Insurers can analyze feedback from surveys, social media, and direct interactions to gauge sentiment. This data can then be used to identify areas needing improvement. For example, if many customers express frustration with a particular aspect of the claims process, that becomes a priority for operational review and adjustment. Tracking satisfaction metrics over time shows whether changes are having a positive effect. This continuous feedback loop is key to ongoing improvement and maintaining a positive customer experience.
Operational Efficiency and Cost Management
When we talk about running an insurance company smoothly, operational efficiency and keeping costs in check are pretty high on the list. It’s not just about making money; it’s about how well the whole claims machine works. Think of it like a well-oiled engine – everything needs to run just right to avoid breakdowns and unnecessary expenses.
Optimizing Claims Adjuster Performance
Claims adjusters are the frontline workers, and their performance directly impacts both efficiency and cost. We need to make sure they have the right tools and training. This means looking at how quickly they can assess damage, how accurately they set reserves, and how well they communicate with everyone involved. Better adjuster performance means faster claim settlements and fewer disputes. It’s about giving them the support they need to do their job well, which ultimately saves the company money and keeps customers happier. We can track things like average claim handling time, the accuracy of initial reserve estimates, and the number of claims that go to litigation. These metrics help us spot where adjusters might need more support or training. For example, if a particular adjuster consistently underestimates repair costs, we know where to focus our coaching efforts.
Managing Reserves and Financial Exposure
Reserves are essentially the money set aside to pay for claims that have happened but haven’t been fully settled yet. Getting these numbers right is super important. If reserves are too low, the company might not have enough cash to cover its obligations, which is a big financial risk. If they’re too high, it ties up capital that could be used elsewhere. Data analytics helps us get a much clearer picture of potential future payouts. By looking at historical data, claim trends, and even external factors like economic conditions, we can build more accurate reserve models. This helps us manage our financial exposure much more effectively and ensures we have adequate funds for future claims.
Identifying Operational Bottlenecks
Every process has its slow spots, its bottlenecks. In claims, these could be anything from delays in getting necessary documents from a claimant to slow turnaround times from repair shops or medical providers. Analytics can shine a light on these issues. By mapping out the entire claims journey and tracking how long each step takes, we can pinpoint exactly where things are getting held up. Once we know where the problems are, we can start fixing them. This might involve streamlining paperwork, improving communication channels with third parties, or even automating certain parts of the process. Getting rid of these bottlenecks makes the whole operation run faster and smoother, which cuts down on costs and improves the customer experience.
The claims process is where the rubber meets the road in insurance. Making it efficient isn’t just about saving money; it’s about fulfilling the promise made to policyholders when they bought their insurance. When claims are handled quickly and fairly, it builds trust and loyalty, which is invaluable for any insurance business. Focusing on operational efficiency means looking at every step, from the initial report of a loss to the final payment, and asking how it can be done better, faster, and more cost-effectively.
Here’s a look at some key areas where analytics can help:
- Claim Cycle Time: Tracking the average time from claim initiation to settlement. Shorter cycles usually mean lower costs.
- Reserve Accuracy: Comparing initial reserve estimates to final settlement amounts to gauge adjuster performance and improve future estimations.
- Litigation Rate: Monitoring the percentage of claims that end up in court. A high rate often indicates issues with claim handling or dispute resolution.
- Fraud Detection Savings: Quantifying the amount saved by identifying and preventing fraudulent claims. This directly impacts the bottom line.
Regulatory Compliance and Claims Data
Insurance is a field that’s watched pretty closely by regulators, and for good reason. They want to make sure everyone’s being treated fairly and that companies have the money to pay out when something bad happens. Claims data is right in the middle of all this oversight. It’s not just about paying claims; it’s about doing it the right way, according to the rules.
Ensuring Fair Claims Handling
This is a big one. Regulators expect insurers to handle claims promptly and fairly. That means investigating properly, communicating clearly with the policyholder, and making decisions based on the policy terms and the facts. If an insurer is seen as acting in bad faith – like unreasonably delaying or denying a valid claim – there can be serious consequences. Analytics can help here by flagging claims that might be taking too long or showing patterns of unfair treatment. It’s about making sure the process isn’t just efficient, but also ethical. Independent adjusters often play a key role in these investigations, looking for any red flags that might indicate a problem [e360].
Reporting and Audit Readiness
Insurers have to report a lot of information to regulators, and claims data is a huge part of that. This includes data on claim frequency, severity, types of losses, and how claims are being handled. Being ready for audits means having clean, organized data and clear processes in place. Analytics tools can help automate much of this reporting, making it more accurate and less of a headache. It also means being able to quickly pull specific data sets if regulators come knocking. This helps demonstrate that the company is operating within the established guidelines and that its rates are fair and non-discriminatory [4147].
Navigating Bad Faith Allegations
Allegations of bad faith can be incredibly damaging to an insurer, both financially and reputationally. These claims often arise when a policyholder feels the insurer didn’t act honestly or fairly. Claims data, when analyzed properly, can help identify potential issues before they escalate. For example, looking at patterns in claim denials, settlement offers, or communication logs can reveal areas where the company might be falling short of its good faith obligations. Proactive analysis can help prevent these situations by highlighting where processes might need improvement or where adjusters might need additional training. Ultimately, good faith handling is a foundational obligation in insurance relationships.
Challenges and Considerations in Claims Analytics
While the benefits of claims data analytics are clear, implementing and scaling these initiatives isn’t always straightforward. Several hurdles can slow down progress or even derail projects if not addressed proactively.
Data Privacy and Security
Protecting sensitive policyholder information is paramount. Regulations like GDPR and CCPA, along with industry-specific privacy laws, dictate how data can be collected, stored, and used. Ensuring compliance requires robust security measures and clear data governance policies. This means not only safeguarding against breaches but also anonymizing data appropriately for analytical purposes and obtaining necessary consents. It’s a delicate balance between extracting insights and respecting individual privacy.
Integration with Legacy Systems
Many insurance companies still rely on older, complex IT systems. Integrating modern analytics tools and data pipelines with these legacy systems can be a significant technical challenge. These older systems might not be designed to handle the volume or velocity of data required for advanced analytics, leading to performance issues or data silos. Often, a phased approach or middleware solutions are needed to bridge the gap, which can be time-consuming and costly. Getting data out of these older systems in a usable format is often the first major hurdle.
Talent Acquisition and Skill Development
Building a successful claims analytics function requires a blend of skills. You need data scientists who can build models, data engineers who can manage data infrastructure, and domain experts who understand the nuances of the insurance claims process. Finding individuals with this specific combination of skills can be difficult. Many companies opt to upskill their existing workforce through training programs, which is a more sustainable long-term strategy. Developing a culture that values data literacy across all departments is also key.
- Data Governance: Establishing clear rules for data ownership, access, and usage.
- Data Quality Management: Implementing processes to clean and validate data before analysis.
- Ethical AI Use: Developing guidelines for the responsible application of AI and machine learning in claims.
The journey to effective claims analytics is often more about organizational change and strategic planning than just the technology itself. Overcoming these challenges requires a clear vision, strong leadership support, and a commitment to continuous improvement. Without this, even the most sophisticated tools will struggle to yield their full potential.
The Future of Claims Data Analytics in Insurance
The insurance landscape is always shifting, and how we handle claims is no exception. Looking ahead, claims data analytics is set to become even more central to how insurers operate. We’re moving beyond just reacting to claims; the future is about anticipating and preventing them.
Emerging Technologies and Trends
Several key technological advancements are shaping the future of claims analytics. Think about the increased use of AI and machine learning, which are getting much better at spotting patterns that humans might miss. This means faster fraud detection and more accurate predictions about claim severity. We’re also seeing a rise in telematics and IoT devices, providing real-time data that can help prevent losses before they even happen. For example, a smart home sensor detecting a water leak could alert the homeowner and the insurer, potentially stopping a major claim before it starts. The integration of these technologies will fundamentally change how insurers manage risk and interact with policyholders.
Proactive Risk Management Strategies
Instead of just processing claims after an event, the focus is shifting towards proactive risk management. By analyzing vast amounts of claims data, insurers can identify trends and potential risks within specific policyholder groups or geographic areas. This allows for targeted interventions, like offering risk mitigation advice or adjusting policy terms before a loss occurs. For instance, if data shows an increase in roof damage claims in a certain region due to aging infrastructure, an insurer might proactively offer incentives for roof inspections or replacements. This approach not only reduces claim payouts but also helps policyholders avoid damage and disruption.
The Role of AI in Claims Transformation
Artificial intelligence is poised to revolutionize the entire claims process. AI-powered tools can automate many of the manual tasks involved in claims handling, from initial data intake and document analysis to damage assessment using image recognition. This frees up human adjusters to focus on more complex cases and customer interaction. AI can also analyze unstructured data, like adjuster notes or customer communications, to identify sentiment and potential issues early on. This leads to a more efficient, consistent, and customer-friendly claims experience. The goal is to make the claims process as smooth and fair as possible, potentially even using alternative dispute resolution methods more effectively when disagreements do arise.
Wrapping Up: The Power of Claims Data
So, we’ve talked a lot about how claims data isn’t just a bunch of numbers. It’s really the story of what happens when insurance meets the real world. By digging into this data, we can spot trends, figure out where fraud might be happening, and generally get a better handle on things. It helps make sure the whole system works better for everyone, from the people paying premiums to the companies providing coverage. It’s not always simple, but using this information smartly can really make a difference in how insurance operates.
Frequently Asked Questions
What exactly is claims data analytics?
Claims data analytics is like using a detective’s magnifying glass on all the information gathered when someone files an insurance claim. It helps insurance companies understand patterns, spot problems, and make things run smoother.
Why is looking at claims data so important for insurance companies?
It’s super important because claims are where the insurance company really does its job. By studying this data, they can figure out if they’re charging the right price for policies, if people are being honest, and how to handle claims faster and better.
How do insurance companies get the data they need for analytics?
They collect it from all sorts of places! This includes the initial claim report, details about the damage, what the person said, repair bills, and even police reports if needed. It’s like gathering all the puzzle pieces.
Can analytics help stop insurance fraud?
Absolutely! By looking at lots of claims, computers can spot unusual patterns that might mean someone is trying to cheat the system. This helps insurance companies catch fraud and keeps costs lower for everyone else.
How does analyzing claims data make the claims process better for customers?
When companies understand claims better, they can speed up how quickly they pay people back. They can also use this knowledge to make sure each person gets treated fairly and to offer better service throughout the whole process.
What kind of new technologies are being used in claims data analytics?
Things like artificial intelligence (AI) and machine learning are becoming big helpers. They can look at huge amounts of information very quickly, find hidden connections, and even predict what might happen next with a claim.
Are there any difficulties when using claims data analytics?
Yes, there can be! Keeping customer information private and safe is a big deal. Also, sometimes old computer systems don’t work well with new tools, and finding people with the right skills to do this kind of analysis can be tough.
What’s the future of using data to understand insurance claims?
The future looks like using data to be even smarter and faster. Instead of just reacting to claims, companies will use insights to help prevent problems before they happen and make the whole experience smoother and more helpful for policyholders.

